Statistics and remarks from health officials in different parts of the state suggest Wyoming is at a pivotal moment in its battle with COVID-19, and has arrived there without significantly bolstering hospital bed capacity.
The federal government gave Wyoming $1.25 billion in the early spring to respond to COVID-19. In a May special session, the Wyoming Legislature authorized the governor to distribute that money.
But a”cumbersome” process of allocating the funds to hospitals means many have started but not completed construction projects to create more capacity for COVID patients, according to Eric Boley, the director of the Wyoming Hospital Association.
“We’ve missed some great opportunities to really shore up and to strengthen our healthcare facilities and providers in our state,” Boley told a legislative committee Tuesday.
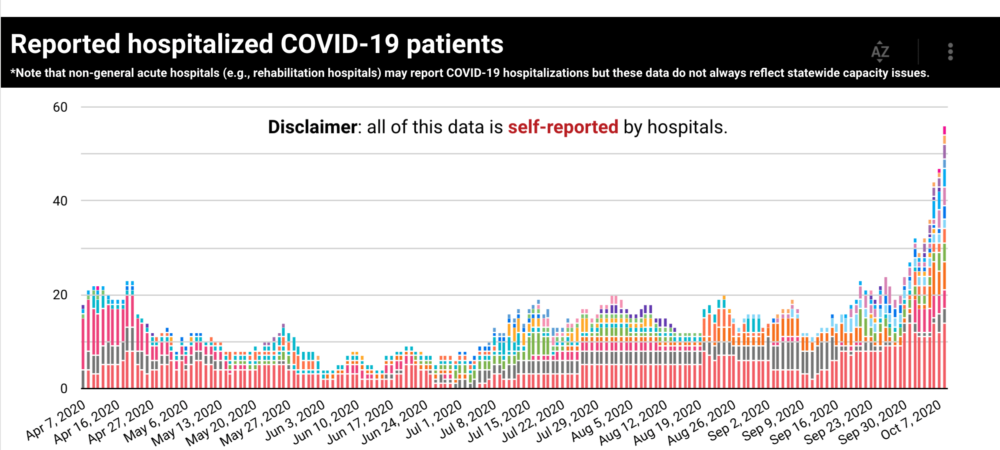
Following a surge in new cases that began in mid-September, the state is now reporting record COVID-19-related hospitalizations.
On Thursday, the Wyoming Department of Health reported there were 56 hospitalizations in the state. However, that data did not include St. John’s Health in Jackson. That hospital reported 9 hospitalizations as of Oct. 8.
Officials at small hospitals worry about their ability to maintain COVID-19 patients isolated while also providing other critical medical services.
Eight people with COVID-19 had come into the ER at Star Valley Health in Afton this week, marketing director Jodi Hill said. The eight patients did not need to be hospitalized and were isolating at home, Hill said, but the sudden influx was a sign of the virus’ increasing presence in that rural area.
Star Valley Health received around $1 million in CARES Act funds from the state government to build nine new reverse isolation rooms, where an infectious patient can be contained. The money was for a new HVAC system to improve air flow in the hospital, plus other safety measures, Hill said. Those construction projects are underway but not complete, she said.
The hospital currently has three isolation rooms.
For now, Star Valley Health will continue to transfer any COVID-19 patients needing hospitalization to larger facilities in other states. The hospital has transferred eight COVID-19 patients over the course of the pandemic, Hill said.
A reliance on out-of-state transfers
Wyoming’s virus numbers are rising alongside those of nearby states. Hospitals in Utah, Idaho and Montana are receiving waves of COVID-19 patients and in many cases are at or nearing capacity, officials say.
Officials from St. John’s spoke to counterparts at larger hospitals in Idaho Falls and in Salt Lake City on Wednesday, St. John’s Health’s Chief Risk and Compliance Officer Dr. Richelle Heldwein said. Both hospitals are still accepting patients, but both report growing capacity pressure.
In Idaho Falls, COVID spread among hospital employees, leading to a staffing shortage, but the hospital remains open to Wyoming patients. The University of Utah hospital in Salt Lake City, where St. John’s and other western Wyoming hospitals can direct patients, is at 100% capacity for COVID-19 patients, Heldwein said.
However, the hospital is building more capacity for COVID-19 patients, and officials there told St. John’s they’re still taking COVID transfers, Heldwein said.
The University of Utah Hospital has 40 inpatients with COVID-19. Officials there predict that count reaching 70-80 patients before “their surge” is over, Heldwein said, “which will completely tax their system.”
These developments could be worrying for Wyoming officials eyeing their own rising hospitalizations and limited bed capacities. “We’re keeping very close tabs on that on a day-to-day basis,” Heldwein said.

St. John’s CEO Paul Beaupre predicted the virus will reach Teton County health workers in an impassioned blog post. He pleaded in the Oct. 2 post for residents to maintain masking, social distancing and other health measures.
“This trajectory is simply not sustainable,” Beaupre wrote.
“We are now all-hands-on-deck to keep the hospital staffed,” he wrote. “With our best effort, we can keep our heads above water today.”
If bigger hospitals stop accepting transfers, St. John’s — and presumably other western Wyoming hospitals — would be left to their own resources. Heldwein could envision the hospital’s 20-some ICU trained nurses working back-to-back shifts to care for a surge in COVID patients there.
“We would make it work, but we would be like New York and New Jersey,” she said, referring to harrowing tales of stressed hospitals in those states during the virus’s initial wave in the United States.
Another large hospital Wyoming relies on, in Billings, Montana, has recently transferred some patients back to Wyoming as it reaches bed capacity due to sharp rises of COVID-19 infections in Montana, State Health Officer Dr. Alexia Harrist said at a Monday press conference.
The state’s long-running fears about an overwhelming pressure on its rural hospitals are crystallizing eight months into the pandemic, Harrist said.
“We are now starting to see those concerning trends that we have been trying to prevent all along,” she said. “Now is the time that we have to turn those trends around.”
The state’s hospitals have not yet been overwhelmed by COVID-19 patients. However, the overall hospital bed capacity has not changed since the arrival of the virus, according to Department of Health data.
The state’s hospitals have more ventilators and more supplies than they had in the pandemic’s early days, Boley, the director of the Wyoming Hospital Association, told WyoFile. “We could make more capacity [for COVID hospitalizations] if necessary,” he said. “In the case of a surge, we have personal protective equipment and other equipment that we didn’t have back in April.”
Hospitals around the state are currently building new bed capacity and new isolation rooms that can hold COVID-19 patients, Boley said. To be reimbursed with CARES Act money, those projects need to be completed by the end of the year, he said. But state officials didn’t award hospitals the funds until mid-July, and many hospital administrators weren’t willing or able to make expensive investments without knowing they would be reimbursed, Boley said.
The pandemic’s early closures inflicted heavy damage on hospital finances, as facilities were forced to cut off elective procedures that generate revenue.

The governor’s office has allotted $67 million in federal CARES Act money to “health care system fortification,” and another $100 million to contact tracing and testing. In the first category, the state has only paid around $414,000, to a Sweetwater County health facility, Wyoming State Auditor Kristi Racines said. State officials, however, have approved a much larger sum, and expect to distribute more in coming months as hospitals finish projects and invoice the state, she said.
The state has spent around $17 million on contact tracing and testing, Racines said. Gov. Mark Gordon on Monday announced that the Wyoming National Guard has been called in to aid with contact tracing as testing confirms a record-breaking spike of new cases.
CARES act funding for business relief has moved much faster. The state had pushed out nearly all of the $325 million allotted as grants for the state’s businesses, Racines said. The concern Boley raised this week wasn’t the first example of officials outside the governor’s administration questioning the pace of CARES Act spending in Wyoming.
“Our ability to treat these patients could have been enhanced and built,” Boley said. “We could have used this funding the way that I think it was intended to.”
The state is at a critical time now, Boley said. “We haven’t peaked and we haven’t started down the other side,” he said of the battle with the virus.


I live in Campbell County, a red zone county now for Covid-19. Our county and city government does not even wear masks, nor require the public to. How can citizens be told to do something when it’s leaders do not? Ridiculous. It’s mostly still considered a hoax or if you do mask up you are sneered at as if you are “ridiculous” or a “liberal”. I’m an RN and take every precaution for my family and patients, even in my off time. This pandemic has become politicized and the death toll will firmly set at the feet of the lack of leadership that has trickled down from Washington to Main Street Wyoming. It’s a shame. Please look out for yourself and family, it’s very simple.
Mixed messages……when this whole thing started WHO, CDC and all the others said masks do not work, we have to shelter in place…….now we have a complete 180.
Here is the problem and its right there in front of everybody. 8 people in Afton show up at the ER with Covid 19 – that’s supposed to scare everybody – but all 8 are sent home to quarantine. Sounds to me like they should not have been at the ER to begin with except for the fact they were probably terrified they had it. But we publicize it as if it’s the end of the world.
There are so many mixed messages, don’t wear a mask, wear a mask, this works, that doesn’t, oh wait, that now works. People are confused, frustrated. I spoke with somebody that was diagnosed and the contact tracers told one group he was exposed to to self quarantine, the second contract tracer told the second group he was in contact with at the same time the exact opposite, they did not need to quarantine. Until the so-called experts/scientists/politicians can get on the same page with the same apolitical message, this cluster will continue. So many people want to make this a republican vs democrat issue, Trump vs the world. Stop, get on the same page and do the right thing, not the political thing.
There is no confusing info in regards to wearing masks….they are proven to help limit the transmission of the virus considerably. It real simple….wear the mask!
The State and Gov Gordo also allocated $ 100 million of that CAREs money to the rural broadband internet program . Just sayin’…
How’s about this – wear a mask! ! Should’ve been mandatory from the get-go but just not “the Wyoming Way” or part of the much-ballyhooed baloney Code of the West. Well, those two Wyoming fables are responsible for a large number of the state’s covid cases. But “wear a mask” can no longer be a mandate here, that horse left the barn six months ago thanks to Wyoming’ s state administration fighting a pandemic “the Wyoming Way”.
Thank you! So simple!
Yes, it is that simple!!!
One thing to keep in mind about “first they said masks don’t help, but now they do…”. Back when this all began, there was hysteria. Even toilet paper was scarce. Masks were even scarcer. Imagine how hard it would have been for vital services like first responders and health care workers to have masks available if the word on the street was “wear a mask or you’ll get COVID?”
Exceptional reporting! Thanks
Wondering what additional measures school districts could take to help slow the spread?
Our Teton County school district board is heavily in favor of keeping schools open. And they don’t see schools as a cause of Covid spread.