A coalition of Wyoming employers aims to find out the true price of healthcare, and the effort may not rely on hospitals and insurance companies for the information.
Instead, the Wyoming Business Coalition on Health seeks private and public employers interested in “pooling” data on their healthcare costs, so they can see how much everyone is paying for hospital procedures and doctor visits around the state.
Armed with data on prices — and a large population of workers who use Wyoming’s hospitals and clinics — employers will have the capability to negotiate prices directly with healthcare providers. The information also will place employers in a better position to demand “bundled” payments — that is, paying a lump sum for common procedures like hip or knee replacements — from the initial visit all the way through surgery and rehabilitation.
The bottom line is Wyoming hospitals are facing a new era when some of their best-paying customers are demanding price transparency and lower costs for healthcare.
“The more costs can be transparent, and we can see how costs are set, the better,” said Kelly Weidenbach, director of Natrona County Public Health, who shared her personal views on the issue. “You can’t have a capitalistic system if customers can’t see prices and shop around.”
High healthcare prices
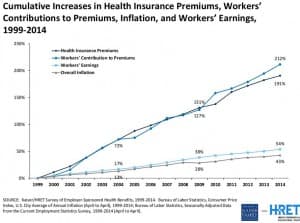
Employers and employees across the nation see their healthcare costs grow steadily, sometimes by 10 percent a year. That is particularly true in Wyoming. The state with the smallest population has some of the highest health insurance premiums in the nation, according to data from the Kaiser Family Foundation.
The rising health costs cut into the earnings of private companies, and the budgets of local governments. “Employer health costs are going up faster than inflation,” said David Newman, a doctor and panelist at a recent conference sponsored by the Wyoming Business Coalition on Health. “Employers can pay more wages, or benefits, but not both. Wages stagnate because employers would rather invest in healthcare.”
As employers seek ways to lower healthcare costs and get better value for what is spent on health care, it places pressure on hospitals. That’s because hospitals regularly use revenue from private payers (employers and their insurance companies) to cover shortfalls from public payers (Medicaid/Medicare patients) as well as uncompensated care.
In other words, hospitals sometimes cover shortfalls in uncompensated care by charging paying patients more for the same services.
Earlier this month, the State Department of Health released a study commissioned by the legislature that details the dynamics of cost-shifting in Wyoming. The study found that hospitals with “high market power” (little competition from nearby hospitals) tend to have more ability to shift costs. The hospitals with the greatest ability to increase prices to shift costs included, Casper, Cheyenne, Lander, and Riverton, according to the report.
Similar efforts to cut costs by pooling data have happened across the country. Many large corporate employers negotiate for favorable healthcare rates for their employees. For a company like Wal-Mart the savings easily amounts to millions of dollars. The first step, though, is knowing what the costs are.
The Missoula Model for “pooling” healthcare data
At a recent symposium hosted by the Wyoming Business Coalition on Health (WBCH) in Casper, Hal Luttschwager, administrator of the public employee health plan for Missoula County, Montana, showed how shining a light on healthcare prices can bring about significant cost savings.

By pooling health cost data for the 970 employees — and with information shared by other employers — Luttschwager was able to contract directly with hospitals and clinics, ask for bundled payments and, ultimately, save money in the county budget.
“We had limited budgets, and every time we had an increase (in the budget for the county employee health plan), we were pulling out workers from patching potholes,” Luttschwager said. “We can’t drive all our costs into the health plan in lieu of public buildings and services.”
After the county health plan received negative publicity for driving up the county budget, Luttschwager decided to try to take back control over what the county paid for healthcare. Up to that point, the plan used a pricing structure with minimal discounts negotiated between a third party and the local care providers.
“We paid 90 percent of the customary and reasonable fee schedule given to us by the company that we paid the bills to,” Luttschwager said. In other words, he had no way of knowing whether he was getting a good discount or not. “We determined we had to change our strategy from lagging the market to matching or leading the market. We wanted to get our prices down to equilibrium.”
The way to do that, Luttschwager explained, was not to seek out deeper discounts, but to find out what other employers were paying and negotiate for a better deal. He got together with a local corporation, the University of Montana, and the state to pool health cost data. They set up a 501(c)(6) organization called the Montana Association of Healthcare Purchasers to collect the data.
“Instead of just having (cost data for) a few hip or knee replacements a year, we had 400 to show, and we knew the pricing and compared it with hospitals across Montana,” Luttschwager said.
According to HIPAA, the medical privacy law, the data was stripped of all personal information, fed into a database and cleaned of inconsistencies, then provided back to the members.
“Finally we got the results back, and we were paying way more than anyone else in the community,” Luttschwager said. Analysis showed that his employees paid more for the same procedures than did patients who were covered by private insurance companies.

The revelation began a long, slow effort to enter into discussions to negotiate better prices with the local network of healthcare providers. Ultimately the county hired a negotiator who met with all the top-50 providers of care for his employees.
Through negotiations, the county health plan and healthcare providers settled on individual contracts that used the Medicare payment as a baseline, and the county would pay a certain percentage above that for each procedure. Hospitals and clinics had the freedom to say yes or no to the contract, while the county health plan agreed to send its patients to those providers first. Many of the providers were resistant at first, but faced with the prospect of losing business, they often reduced their prices.
Hospitals can sometimes make up for the reduction in prices by attracting a greater number of patients. In the course of negotiating better rates with providers in the county’s network, Luttschwager saw that a number of hospitals in neighboring towns outside of his network lost patients, while the local hospitals in Missoula gained.
“It’s like playing poker, where you know all of your cards and four of theirs,” Luttschwager said. “We dump all the data into the warehouse we can, and ask for the data we want back. We plug in codes for mammography, compare them, talk to the providers to say, ‘We have a good provider in you and we (provide you with a lot of business), can you work with us?’ We can look at the data, and say ‘your mammogram is ten bucks higher than someone else.’ They may not know that.”
That last part is worth noting: Medical billing is so complex that hospitals sometimes don’t know precisely what it costs them to cover the medical expertise, supplies, and overhead for a certain procedure.
Armed with the pricing data and the ability to negotiate with providers, the growth of spending on the Missoula County health plan has leveled off.
“We saved over a million and a half dollars by going to a Medicare-based (price) schedule negotiated with us,” Luttschwager said.
That, in turn, kept county employees from having to pay in more to the plan. “This year was a zero rate hike. I haven’t been able to say that in a long time.”
Luttschwager has also been able to spot high-cost trends in the data, like the price of rehab for patients addicted to narcotic pain-medications. This resulted in a policy restricting patients’ access to pain meds after a certain amount of time after a surgery. He’s also able to track particularly high-cost cases and strategize on how to manage those cases in a more economical way.
Despite all the negotiations with local providers, Luttschwager says county employees can still seek out-of-network care if they choose.
“We allow patients to go anywhere they want, but they pay the difference,” Luttschwager said.
“Bundling” costs in Wyoming
By pooling data, employers have the opportunity to see what procedures are happening routinely and then begin negotiating with providers for a new payment structure. For high-volume procedures like hip or knee replacements, employers can easily track how much they are spending, and then negotiate for an all-inclusive rate — or “bundling.”
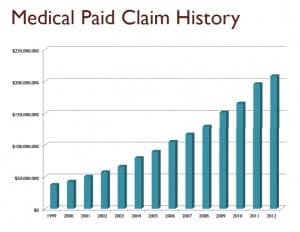
A bundled rate may cover a certain time period before and after a procedure, or even all the medical care from the first x-ray to the last session of physical therapy.
About a year ago, the Wyoming Business Coalition on Health (WBCH) heard from a Wyoming hospital that it was interested in working with employers who wanted to bundle payments. That caught the coalition off-guard, because it had no data on what they should be paying for bundles.
“With pooled data we can expose the price variation, and with a bundled payment you provide an incentive to the delivery system to squeeze out unnecessary procedures,” said Anne Ladd, director of the WBCH. “Then we put the delivery system on notice that, ‘I don’t mind paying the right amount for a neck surgery when it is needed, but I don’t want to pay for it when it is not needed.’”
(Full disclosure: Ladd is a board member of WyoFile.)
An important feature of bundling is that employers can strike a deal to pay for a procedure once, but if the procedure fails and results in a readmission due to medical error, the provider agrees to cover the cost. This puts a heavy incentive on the hospital and doctors to get a treatment right the first time.
“Our first shot through our heart valve bundle, we saved $145,000 because we had a readmission and the hospital ate the cost,” Luttschwager said.
In negotiating bundles, he says he is careful not to push the price too low. “I left a little money on the table because I wanted this to work. I wanted the warranty to work for them (the providers). They determined what was in the bundle after we said we want start to finish.”
Bundles only work in certain cases with a relatively good prognosis. The county avoids bundling for patients with chronic diseases that could result in complications.
“Bundles are just a little piece of the whole thing,” Luttschwager said. “Direct contracting was the big dollar saver.” He noted the problem with pushing down the price of a bundle too much is that it can push the price up for other services to make up the difference — another type of cost-shifting.
Dr. David Newman, a panelist at the WBCH event, emphasized that bundled payments don’t guarantee reduced costs. He cited an analysis by Princeton University economist Uwe Reinhardt.
Even so, bundling can provide a major incentive to doctors to rein in costs, because they don’t want to exceed the payment offered in the bundle. This helps reduce use of costly and unnecessary medical devices, like cold water circulating tanks for knee rehab that can be replaced with ice packs that cost $2. With bundled payments, doctors start looking at the bottom line and calculating where costs can be saved.

It’s uncertain whether bundles will work in Wyoming, because they function best in competitive health markets like Missoula, where the employer has two hospitals and many specialist clinics to choose from. That allows the employer leverage in negotiating prices. With most towns in Wyoming having one hospital, this may not work as well, though some areas in the state have enough regional hospitals to provide competition.
“We have a medical drain around the border,” said Rep. Elaine Harvey (R-Lovell) who attended the WBCH conference and co-chairs the Legislature’s Health, Labor, and Human Services committee. “It is difficult to build a medical system in Wyoming. For me personally it is 90 miles to Billings, Montana, and 240 for me to come to Casper. For convenience sake, if my husband was in the hospital, I’d rather go 90 miles than 240.”
The bigger question may be whether Wyoming hospitals will respond to healthcare price negotiations in a way that makes them competitive with out-of-state providers.
State unlikely to take on data pooling
High healthcare costs also affect the state budget. Wyoming spent $208 million on its public employee health plan in 2012, with the state covering more than 80 percent of the cost of care, and employees paying the rest. The total group plan covers some 37,000 lives, including state employees and their families, employees of the University of Wyoming, community colleges, and Natrona County School District 1, and retirees.
Based on comments by Rep. Harvey, it may be a challenge to convince the state to join an all-claims database to pool health data. She said several other states have these, but many are now moving away from such large-scale data collection.
“We have been toying with an all-claims database,” Harvey said. “They are expensive, they don’t work, and they don’t get to the questions we are looking at.” Harvey said she learned about other states’ experiences with such databases at a recent National Conference of State Legislatures meeting.

Dept. of Health Director Tom Forslund says that too often the Legislature directs agencies to collect data that isn’t fully used. “At the end of the day, who is going to use it, and how are they going to use it?” Forslund said. “What problem are you trying to solve? You have to know that before you start to grab the data and analyze it.”
Ralph Hayes, the administrator of the Wyoming’s Employee Group Insurance plan, says his program is in the early stages of working with its data. He recently hired an analyst in hopes of getting a better handle on how to reduce costs. Hayes says he has good information to identify high-cost areas, “But I still don’t know where I stand as far as everybody else.”
Employers don’t necessarily have to rely on the state to join their effort, according to the WBCH. Coalition representatives say there may even be a better alternative than a state-based health data system: a non-governmental group to collect data from public and private employers.
The Montana Association of Healthcare Purchasers has already built the infrastructure for collecting such data, and it is possible Wyoming could use the same system. The WBCH could then contract with a company in Helena, or another similar consultant, that has the expertise to vet and analyze data and send it back to Wyoming employers.
“We are hoping we can put together a voluntary claims database to start putting together the data and start a pilot project to see if we can negotiate with hospitals and make it work,” said Ladd, director of the WBCH. “In the absence of having our local insurance carriers cooperate with us (on sharing data), we have us. That’s the other option.”
Newman, the doctor who participated as a panelist at the WBCH event, said the day’s discussion represented a good introduction to the potential of aggregating health data, not just for the benefit of businesses, but for the whole state.
“It becomes an economic argument for growth of Wyoming, and businesses wanting to look at Wyoming as a place to come if costs are reasonable,” Newman said.
Click here to see the membership of the WBCH.
For more WyoFile coverage of healthcare issues, read these articles:
“Governor candidates weigh options for Wyoming Medicaid expansion,” September 2014
“Health and finances are uncertain in Wyoming’s Medicaid gap,” September 2014
“‘Medicaid expansion still very important’ on reservation,” July 2014

