Wyoming reached a critical point in its battle with COVID-19 this week as patient loads overwhelmed hospitals, healthcare workers and contact tracers, prompting the governor to announce plans to tighten health orders for the first time since spring.
Virus infections continued to snowball as the rate of spread accelerated for a tenth straight week. New daily lab-confirmed cases obliterated previous records, active cases grew by 57%, surpassing 8,000, and hospitalizations reached a new peak of nearly 200.
Gov. Mark Gordon, who just emerged from quarantine himself, sounded the alarm during a press conference Friday, saying he is “concerned and angry” about the situation. Wyoming is among the states experiencing the most severe outbreaks in the pandemic-beleaguered nation.
“Our state is at a fever pitch,” Gordon said.
Hospitals are so desperate they are erecting tents, businesses are forced to close due to outbreaks and more people are dying, Gordon said. He sharply admonished people to take health precautions like mask wearing and social distancing seriously.
“Our capacities are overwhelmed,” he said. “It’s time that Wyoming woke up and got serious about what it’s doing … because we are being knuckleheads about this … We’ve relied on people to be responsible, and they are being irresponsible.”
The situation is so critical that state officials plan to tighten health orders for the first time since the spring, Gordon said. He declined to elaborate on particular orders, but said a mask mandate is not off the table.
“There will be changes,” he said. “They will be more restrictive. We are looking at every aspect of what we can do.”
Health officials expect the situation to deteriorate, he said.
Widespread Infections forced the closure of several government buildings, and the state adjusted nearly all of its metrics to “concerning.” Some schools have announced transitions to online education, and hospitals report severely strained staffing.
The state this week announced 22 COVID-19-related deaths, bringing the toll to 127. More than half of all deaths, 55%, have been announced since Oct. 17. Among those being mourned is Rep. Roy Edwards (R-Gillette), the state’s first known public official to die of COVID-19.
The volume of new cases has become so overwhelming that the Department of Health has scaled back its contact tracing. Where the department previously attempted to contact individuals who tested positive as well as known close contacts, it has shifted its priorities.
“We will focus now on following up in a timely manner with residents who have tested positive,” Dr. Alexia Harrist said in a Tuesday release. “Close contacts may also receive calls at times from public health representatives, but only in certain priority situations and settings.”
Instead, the DOH is instructing infected people to notify close contacts themselves.
County health offices are also struggling to keep up. Teton County Director of Health Jodie Pond told the Jackson Hole News&Guide her department was forced to make truncated contact tracing calls after being swamped.
“We are triaging,” Pond said.
All told, Wyoming has now tallied 17,442 lab-confirmed infections.
That includes 4,488 new cases in the last week — the largest weekly growth by far — nearly double the previous record. New single-day infections also shattered records, with 917 reported Nov. 6 followed by 1,171 reported Tuesday and 924 Thursday. The previous record, set Oct. 30, was 431.
By Friday morning, active cases — the number of people officials believe are fighting infections but haven’t recovered — reached 8,767, a 57% increase from last week.
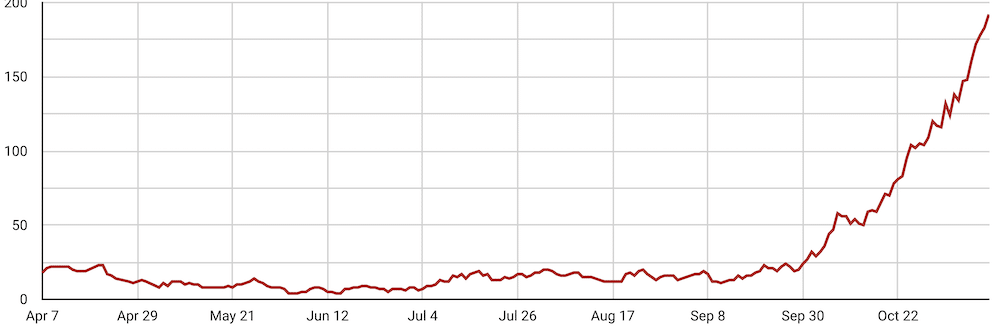
The number of statewide hospitalizations reported by the DOH hit a new record of 192 Thursday. That’s a 264% increase from a month ago on Oct. 12.
In response to staffing shortage concerns, Gordon announced Wednesday he will use $10 million in federal relief funds to bring temporary medical personnel to Wyoming.
“Medical staff across the state are strained and exhausted,” Eric Boley, President of the Wyoming Hospital Association, said in a release. “There is an immediate need to bring in additional help to ease the burden shouldered by our healthcare professionals.”
When asked where he will find additional personnel as healthcare needs mount across the country, Gordon on Friday acknowledged that it will be difficult, and likely expensive.
Wyoming residents are reporting more anxiety as the surge stretches into a third month, according to the latest survey by the University of Wyoming’s Wyoming Survey and Analysis Center.
Almost half of Wyomingites say they’re very or fairly anxious about the spread of COVID-19 in the state, an increase of 8 percentage points from October and 15 percentage points from September, according to WSAC.
Support independent reporting — donate to WyoFile today.
“Anxiety about the spread of COVID-19 in Wyoming has returned to levels not seen since March,” Brian Harnisch, senior research scientist in charge of the project, said in a release. “At the same time, we see just over two-thirds of Wyomingites now reporting that they are wearing a mask in indoor public places all or most of the time. Other research has shown that this number is still likely the lowest in the nation.”
More than 60% of Wyomingites now say they would strongly or somewhat support an ordinance requiring people to wear face masks in public buildings, according to the survey. Thirty percent say they strongly or somewhat oppose such an ordinance.
Wyoming is not among the 34 states that have issued mask mandates. However, Albany, Laramie, and Teton counties and the Wind River Reservation have enacted mask orders. Natrona County joined this week with an ordinance that mandates mask use in certain county-owned buildings, the Casper Star-Tribune reports.
More than 20 county health officers sent a joint letter to Gordon on Thursday asking for a statewide mask order, the Casper Star-Tribune reports.


Where in Wyoming has a hospital erected a tent? According to the American Hospital Association Data Hub for the week ending Nov 9 the Wyoming hospital capacity utilization was at 42.1%, up only 2.2% from the three year average. Fear mongering with bad data is not helpful.
Public mask wearing has not been shown to reduce the incidence of viral infection. The recent Danish RCT study of mask use showed a minuscule difference between infections in masked or unmasked, (1.8% vs 2.1%) and the Naval Medical Research Center did a careful study of recruits with masks, disinfecting, and distancing vs a control group, and again found a minuscule difference, with the masked infection rate actually higher at 2.8% vs the control group at 1.7%.
Telling the vulnerable they will be safer with masks is an unfounded claim that can make them very sick.
If the hospitals get too full, triage will result in the younger, healthier people who did not believe they would get sick to be preferred over the old and infirm who may have been infected in a nursing home. Seems like those wearing a mask when out in public, for food shopping, doctor appointments, etc., should receive more hospital priority than a deneyor or parent who did not isolate their family when a member became sick.
Since we can’t rely on people to wear masks I think it’s doubtful to rely on individuals to do their own contract tracing. Teachers in our schools are hearing about family members of students (siblings, parents etc) that are testing positive yet their kids are still coming to school. There are many people who still think it’s all a joke and won’t tell anyone they were in contact with about being sick. Parents aren’t even telling the schools when their kids test positive (if they get them tested) so the school can evaluate if any other students or staff should quarantine. Without Public Health doing contact tracing that will just increase the number of people out there spreading it to the 1% that will die from it and countless others that may have long term health issues as a result of just being infected with it.
We know families will gather for Thanksgiving and Christmas, and bars will be full for New Years…no end in sight.
“Concerned and angry” governor? Well so are we the citizens for a complete lack of leadership. Just like our ex-president, all rant with no useful action.
We’ve needed mask mandates for months. If citizens don’t see their responsibility towards others they should go live alone somewhere, perhaps a jail cell? Igloo?
Doing nothing is a complete breach of your oath.
my comment from last week’s covid update article with minor adjustments:
congratulations to all those who feel that wearing a mask is against your civil liberties. your selfishness and ignorance has made our state worse off.