Two Wyoming residents who exhibited symptoms of COVID-19 infection said they fear their experiences of denied testing and delayed treatment demonstrate how scarce supplies and a slow response may have exacerbated the pandemic’s spread.
Both women had fevers, low blood-oxygen levels, coughs and difficulty breathing beginning in late February. One has pre-existing health vulnerabilities, including asthma and heart trouble, and works with vulnerable communities. Both traveled beyond their home towns and had weeks to unknowingly spread contagon. Neither has been tested yet.
The state’s guidelines for testing and its capacity for processing them has changed several times since the two women first showed symptoms similar to those of influenza and COVID-19, Kim Deti, Department of Health spokeswoman, told WyoFile on Wednesday.
Wyoming issues guidelines that physicians use to determine who is tested and who is not. Initially those with travel histories or contact with people known to have been infected were high priority. People seeking testing had to, and still largely must go first to their primary healthcare provider, who decides whether to proceed, she said.
New guidelines issued yesterday prioritize healthcare workers who have been in touch with infected patients and who also exhibit symptoms; patients who are hospitalized; people susceptible to illness; older people and people who live in communal settings, according to the department . Physicians no longer need state permission before submitting a sample for testing, the new guidelines say.
But guidelines are moot without the materials needed to execute the tests, and that’s not the state’s responsibility, according to the DOH. “The [Wyoming Public Health Lab] does not provide swabs or viral transport media,” the guidelines on the Wyoming Department of Health reads.
Some healthcare providers are short of the swabs and transport vials, making it necessary to select patients for testing according to state guidelines.
In a video released this week by the Northern Arapaho Tribe, Dr. Paul Ebert, chief medical officer of Wind River Family and Community Health Center in Arapaho, said testing capacity is limited.
“Despite what you are seeing on TV and what the feds are saying, we still do not have widespread testing available,” Ebert said. “Because we are in a rural area, our testing depends on what’s called viral transport media … there’s a very limited amount of that media available right now.
“Right now we have to pick and choose who we test,” he said.
In Jackson, one physician told WyoFile he ordered 20 sets of swabs and transport vials from LabCorp, and expects to get them in 24 hours. He had only a couple of sets on hand Wednesday, he said, but doesn’t want to deny testing to those who want it.
“We’re doing testing on-demand,” Dr. Brent Blue of Emerg+A+Care said. “If [patients] want to pay the $80 [for the swabs, vials and lab work], we don’t care.
“The average physician probably has two or three sets,” Blue said of the swabs and vials. “We’ve never been told how to get [them] from the state.”
Amy Surdam, who runs Stitches Acute Care Center in Laramie, Cheyenne and Wellington, Colorado, also is short of swabs and vials. “We’re trying to source the supplies from wherever we can,” she told WyoFile.
“We have some right now but it’s still very limited,” Surdam said. “We think we’re going to get more tests today. We have labs that can process more tests than we have swabs.”
Personal protective gear also is in short supply, she said. “We have one mask per staff member — that’s it.”
“Mass testing and mass isolation is how we beat this and we’re not doing either,” Surdam said.
Nationwide and in Wyoming the inability to roll out widespread testing for the coronavirus COVID-19 has generated expansive debate and criticism. Medical workers have tested 251 people of Wyoming’s estimated population of 579,280 residents, the Wyoming Department of Health reported Thursday.
Most of those were completed at the Wyoming Public Health Laboratory; the federal Centers for Disease control analyzed one test and commercial labs another 12. On Thursday morning, the state reported 17 confirmed cases of COVID-19 spread across Fremont, Park, Sheridan, Laramie and Teton counties.
An early case in Lander
It was “like an elephant standing on a lung,” said a 44-year old school district employee in Evanston who asked not to be identified by name for privacy and other reasons. Her problems began on Friday, Feb 29.
A physician disagreed with her assertions that her malady was COVID-19-like and instead ordered tests for blood clots and heart problems. Neither he nor a medical facility instituted what she believed should have been proper hygienic protocols.

The other patient, 64-year-old Lander health care professional, woke up Tuesday, Feb. 25, “with a very hard coughing — a lung kind of cough.” She has other health problems and didn’t initially think she might have been at risk for COVID-19 infection, she said.
But when her symptoms persisted and worsened, she found little help and no test available, despite her vulnerable health profile. She paraphrased one response to her request for testing: “You don’t need it. We just need to assume influenza — the flu.”
She first noticed her symptoms after traveling to Cheyenne the weekend of Feb. 22. While in the capital, she attended functions with large numbers of people and dined out.
It would be 15 more days before Wyoming announced its first confirmed case of COVID-19 in Sheridan County.
Given her ongoing health problems, including asthma, previous heart attacks and other issues, she knew it would take more time for her to recover from what she figured was a flu than it would other, healthier people.
She cut her hours at work and went home early on Friday, Feb. 28. “I was running a fever in the mornings,” she said. “When I woke up I was drenched” in sweat.
Looking back, she said she should have stayed home. “Because I do get sick very easily, I try very hard not to let those things interfere with my work,” she said.
The week of March 2 she worked short hours again. On Friday, March 6, she called in sick, went to a physician and reported her symptoms.
“They gave me a mask,” she said. “They got me through very quickly. I had shortness of breath.” Her blood oxygen levels were lower than normal.
“You have all of these underlying medical conditions,” she paraphrased her physician. “We’re just going to treat you like you have influenza. Come back if you are not better.”
It would be five days before Wyoming would announce its first COVID-19 case. It would be seven days before the state announced the first case in Lander, where she lives.
She kept trying to work
The woman again tried to work the week of March 9, again for short hours and behind the closed door of her office. The Department of Health announced the first case in the state that Wednesday. She went home from work early Thursday. She did the same Friday, the day the state announced the Lander case in a resident of the Showboat Retirement Center.
On Monday, March 16, with a confirmed case in her backyard, she again sought medical attention. “I’ve been sick a long time,” she said she told her physician. “I still have these symptoms. I think I need to be tested for influenza or COVID, or whatever.”
The response was, “you don’t meet the criteria,” without having traveled internationally, she said she was told. Even a call to state officials couldn’t provide a test, she said.The Department of Health referred her back to her physician, she said and, if she had a complaint, to the State Medical Board.
“The way they’re handling this is they’re completely disregarding human nature,” she said. “In this particular case they’ve decided ‘we’re not going to give any information at all.’”
“Just give people some information,” she said. “Don’t treat us like we’re stupid — just be honest with me. Say ‘We don’t have enough tests, therefore we’re going to go ahead and treat you for all the underlying conditions.’”
Evanston to Utah, Denver and back
In Evanston, the school district employee said she began coughing Thursday, Feb. 27, three days after she had contact with a person who had been in contact with the Lander health care worker above, and two days after that patient first noticed her affliction.
She traveled to Salt Lake City and mingled with large groups of people the weekend of Feb. 29. “I just felt a little different, run down,” she said. Her temperature rose to 101.
But she soldiered on. “I really was busy and had a lot of things to do,” she said.
After returning to Evanston, she traveled to Denver and again mixed with crowds. She began seeing stories about COVID-19 and suspected the worst. She returned to Evanston on Tuesday, March 10 and saw a physician the next day.
He came in with no gown or smock or lab coat — “just his Tommy Hilfiger polo shirt on,” she said.
“There was no face mask available,” she said. Her blood-oxygen level was low.
The doctor ordered a blood test, a chest X-ray and an EKG or electrocardiogram to measure her heartbeat. She protested but began going through the tests at a medical center.
Waiting for one procedure, she found herself close to six or seven elderly people. She was coughing into the crook of her elbow.
“I was feeling lightheaded,” she said. “This is not a good idea,” she said she thought to herself. “I called my husband to come pick me up.”
Her physician tracked her down by phone and asked why she didn’t complete all the tests he had ordered, she said.
“I don’t want to get other people sick,” she said she told him. She paraphrased his response: “You might have a touch of the flu — sleep it off.”
The next day, she went back to find out one test was negative for blood clots, she said. By then, March 12, the physician’s procedures had changed. Workers asked her to wear a mask.
Support informing your community — donate today
But when she asked whether she should get tested for COVID-19, the answer was no.
“I have no protocol on that,” she paraphrased the physician. “At this point, there’s not enough tests in Uinta County. We’re saving those for our elderly patients.”
The medical center administrator did call her to apologize for letting her walk around the facility while potentially exposing others to an illness, she said.
“I feel like I’m getting better,” she said Tuesday. “My lungs don’t feel as heavy. I still have a cough. I think my [oxygen] levels are higher. I haven’t had a temperature I’m aware of.”
What’s next?
Health Department spokeswoman Deti said she’s heard no plans for mass testing in affected areas like Lander.
“I don’t know if that’s a capability we will or will not be able to offer,” she said.
Whether anybody who has symptoms can get tested remains the decision of a person’s physician, Deti said.
“Your health-care provider would have to use their judgement,” she said. “If they did [want to test] they would take a swab.”
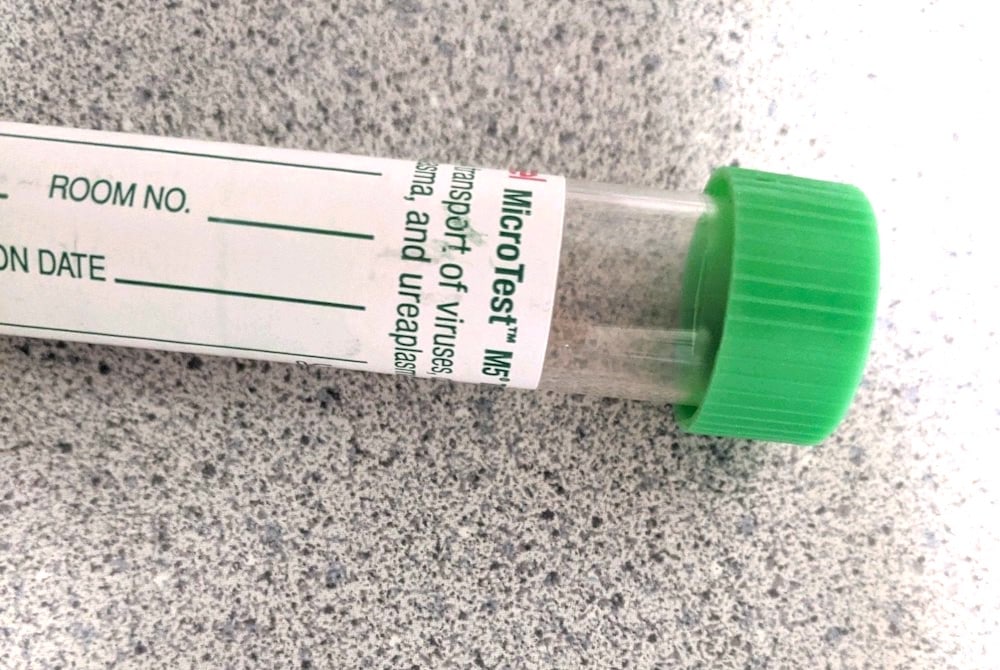
The process involves inserting a long Q-tip-type probe deep into a patient’s nose, then withdrawing it and sealing it in a vial for transport to a laboratory for analysis.
Some local health centers have provided drive-up testing, Deti said, pointing to Cheyenne as one location.
Wyoming opened its own laboratory to COVID-19 testing March. 5. Before that, tests had to be sent to the federal Centers for Disease Control.
If a testing bottleneck still exists, however, it’s not with the state laboratory’s capacity, Deti said.
On a recent day, the laboratory analyzed some 100 swabs from patients’ noses, Deti said. There are 150 or so pending tests entered in the state computer system, meaning a provider has sent samples to the laboratory for processing.
“It’s hard to look back and know what may or may not have happened,” she said of the women’s particular cases. “The testing at the time was limited.”
The state laboratory, “they’ve been keeping up,” she said. “There’s no backlog.”
— Andrew Graham and Katie Klingsporn contributed to this story.



I wholeheartedly agree with Melanie! Excellent reporting Angus & Co. I’m glad I found this article (on March 28th). Has there been a follow-up report on the status of testing?
On a lighter note, as I was reading this it reminded me of my days working as a Ranger in the Bridger Wilderness back in the 80’s. I was hiking alone in the Upper Green River and had a peaceful encounter with a big blond bear on a forested slope on my way up Square Top Mountain. When I tried to talk to Game and Fish about the experience, they were adamant it could not possibly have been a Grizzly. I’m fairly certain it was. Similar reports of Wolverine during that time were rejected too, but now we know they were there all along.
Keep up the good work! –Megan Lyons Bogle, Alta, Wyoming
I’ve been hearing stories like this in Cheyenne and in Denver. We have way more than 24 infected and still Cheyenne Mayor Orr does not order more stringent business closures and precautions! Wyoming Governor better do something and get massive testing implemented ASAP and do whatever is in his power to stop the spread. “Suggesting” is not good enough! Your news is the only news reporting the truth of what is happening here in Wyoming. People here need to start taking this seriously (and there are still many in denial).
I went to Colorado springs on February 20 and spent several hours in a massive group of people. March 5th I had a dry cough, headache, shortness of breath. I called in sick to work Thursday and Friday. That weekend Covid 19 went crazy. I called urgent care in Cheyenne and was told they would not test. I contacted the state health department and was told they would not test. I self isolated and worked from home. After a week of being sick I went to my family doctor. I was told I had something viral, but I could not be tested for Covid because even though I had a sore throat, cough, shortness of breath for over a week, I had type II diabetes and I had been in Colorado Springs in a massive group a month earlier, because I didn’t have a fever while st the doctor’s office, I could not be tested. There could be many more cases than reported in Wyoming, but they will not test for it….unless you can pay $150 to $300 from Everlywell for a home test.
My husband with travel history throughout Wy and CO was also very sick coughing, breathing issues. He missed about 3 weeks of work, going in for a few hours some days. Despite his history, he too could not get a test. Our family has been sick since the last few days of February. I understand now, there was a lack of tests and it’s probably’ ‘just the flu’ (which they did not offer to test). But we’re in Lander where there is evidence of community spread that they can’t track. Also as a family we’ve not been this sick in about a decade. One kid is still spiking 101 fevers.
This dovetails with the report this week that Wyoming ranks dead last among the 50 states and DC in aggressively coping with the Covid-19 situation.
This is one of the scariest articles I’ve read over the past two weeks. If this is the way many medical “professionals” in Wyoming are dealing with this epidemic, in effect actively spreading the virus instead of quarantining suspected cases, we are truly in deep trouble.
Nancy D, you are so right! This is frightening to think about. Dr. Blue, just tested someone in Jackson without symptoms, test came back
Positive. His entire staff, including himself are now being tested. Opening back up on Monday. He has the right idea though. Anyone can be tested at his office that wants to be tested. Fee: 80.00.. at least we know what we are dealing with.
Cathy Newbern
I congratulate Angus on yet another exceptionally well-researched and thorough story about the difficulties Wyoming residents have faced while attempting to get testing, treatment and general care. These stories need to be covered, and Angus’ talent for searching out and writing preventive stories about important issues is exceptional.
Angus performs a great community service in preventive journalism that other news outlets simply don’t. And he does so with a turn of phrase that’s easy and enjoyable to read.
Thank you,
Melanie Harrice
Kelly